How Aware Are You of Peripheral Artery Disease?
September is Peripheral Artery Disease Awareness Month, making it a great time to discuss risk factors for PAD, signs and symptoms, and the importance of getting diagnosed and treated.
What is it?
Peripheral artery disease (PAD) is a condition that can cause leg pain that gets worse with activity. Muscle pain that gets worse with activity and better with rest is called "claudication." PAD affects the blood vessels (called arteries) that bring blood to the legs. PAD can also cause wounds to heal more slowly than usual.
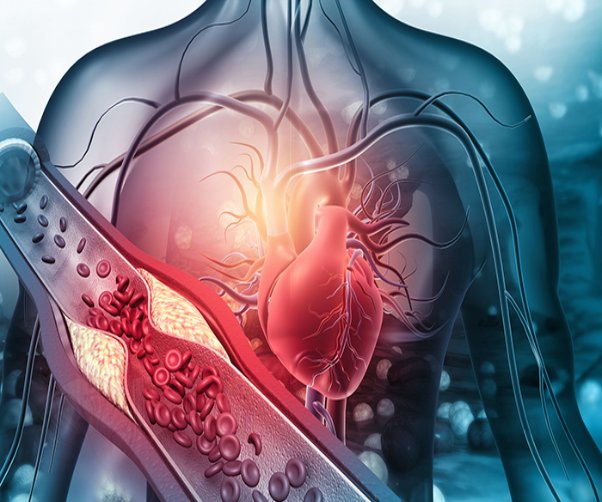
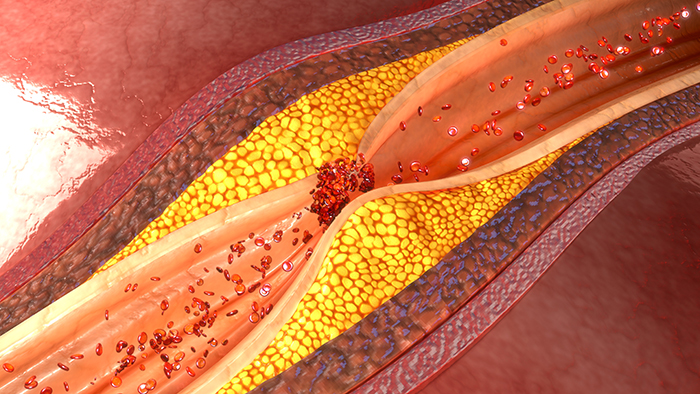
What causes PAD?
Normally, blood flows easily through arteries to all parts of the body. But sometimes, fatty clumps called "plaques" build up inside the walls of the arteries. Plaques can cause arteries to become narrow or blocked. This prevents blood from flowing normally. When muscles do not get enough blood, symptoms can occur.
What are the signs and symptoms?
- Pain in the back of the lower leg. The pain usually gets worse with walking or other exercise and gets better with rest.
- PAD can also cause pain in the buttocks, thighs or sometimes in the feet.
People who have leg pain can have other symptoms, too, such as:
- Trouble walking up stairs
- Trouble getting an erection (in men) or trouble with sexual arousal (in women)
Symptoms of claudication can be mild or severe, depending on:
- Which arteries are affected
- How narrow the arteries are
- How much activity a person does
Risk factors
Some people have a greater chance of getting PAD, such as those who:
- Smoke
- Have diabetes
- Have high cholesterol
- Have high blood pressure
- Are physically inactive
Screening
Your doctor or nurse can do different tests to find out if you have PAD and how severe it is. He or she might:
- Take the blood pressure in your arm and lower leg (just above the ankle) at rest and right after exercise and compare them
- Take the blood pressure in other places in your leg (like the thigh)
- Order a blood vessel imaging test such as an ultrasound, which can show pictures of your leg arteries
SUBSCRIBE TO OUR BLOG
and you'll receive more health & wellness tips right in your inbox.
SUBSCRIBE NOWHow is PAD treated?
If you have PAD, there are things that you can do:
- Stop smoking
- Get your diabetes, high blood pressure, and high cholesterol under control (if you have these conditions)
Some people are also treated with medicines. The medicines used to treat PAD can reduce symptoms, increase blood flow to the legs, and help people walk farther without pain. People who have certain heart problems may not be able to take the regularly prescribed medicines. Your doctor will help determine which medicine is best.
If you still have severe symptoms after trying medicines, your doctor will talk with you about the possibility of having surgery or a procedure to increase blood flow to your legs and feet. Your treatment options might include:
- Angioplasty or stenting – During angioplasty or stenting, the doctor sends a thin tube with a balloon at the end of it to the part of the artery that is blocked. Then the doctor inflates the balloon to open the blockage. Often the doctor props open the artery using a tiny mesh tube called a stent, which stays in the body.
- Bypass surgery – During bypass surgery, the doctor removes a piece of blood vessel (vein) from another part of the body. Then he or she reattaches that piece of blood vessel (called a vein graft) above and below the area that is clogged. This re-routes blood around the clog, and allows it to get to the part of the leg that was not getting enough blood. Sometimes instead of taking a graft from another part of the body, the doctor can use a man-made graft.
What happens if PAD is left untreated?
Leaving PAD untreated can lead to worsening quality of life and the inability to exercise and walk. In severe cases, it can lead to a condition called critical limb ischemia where the limb/foot is threatened and may lead to amputation.
Is there a way to prevent PAD?
You can help prevent PAD by controlling and managing your risk factors. The major risk factors for developing peripheral artery disease include:
- Cigarette smoking - Cigarette smoking is the most significant risk factor for developing PAD.
- Diabetes
- Hyperlipidemia (elevated blood levels of lipids, including cholesterol and triglycerides)
- Hypertension (high blood pressure)
- Physical inactivity
Do you have questions you’d like to ask a healthcare provider?
A primary care provider can meet with you and make an appropriate referral
Related Articles